Regulation of GFR: autoregulation via myogenic mechanism Myogenic mechanism
By: HWC
Date Uploaded: 10/24/2019
Tags: homeworkclinic.com Homework Clinic HWC Regulation of GFR Renal autoregulation Nervous regulation sympathetic neuron juxtaglomerular cells afferent arteriole mesangial cells ascending limb of loop of henle efferent arteriole autoregulation autoregulation via myogenic mechanism Myogenic mechanism vasoconstricting macula densa cells arteriole vasodilates Neural regulation angiotensin II
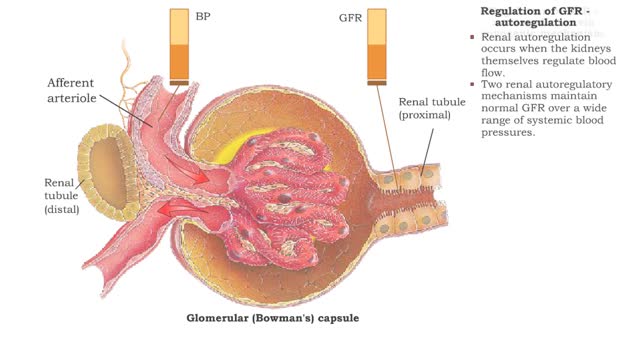
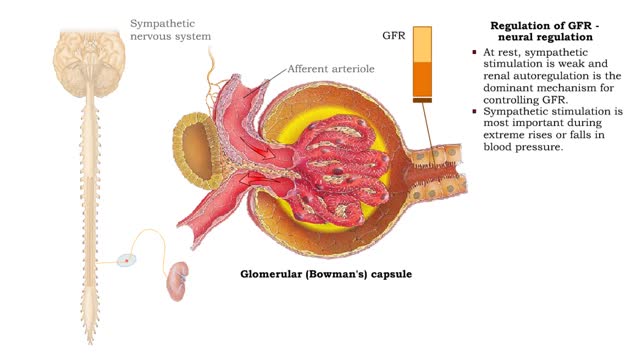
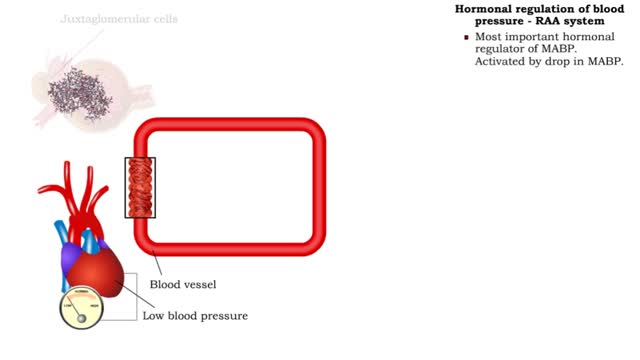
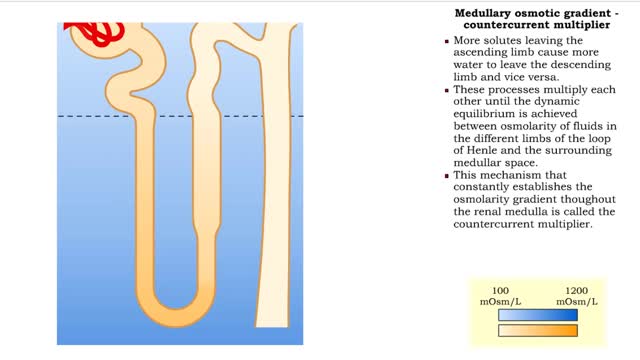
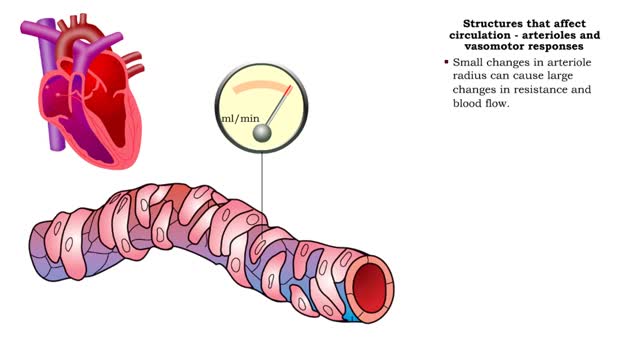
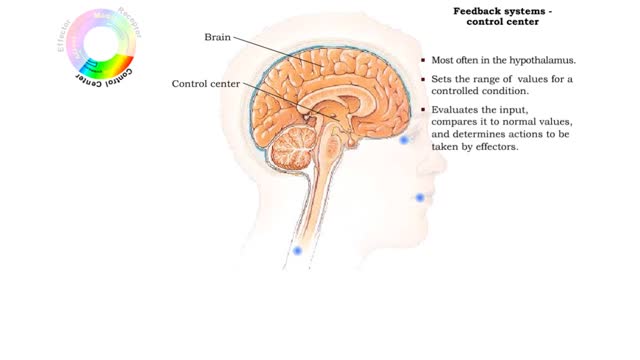
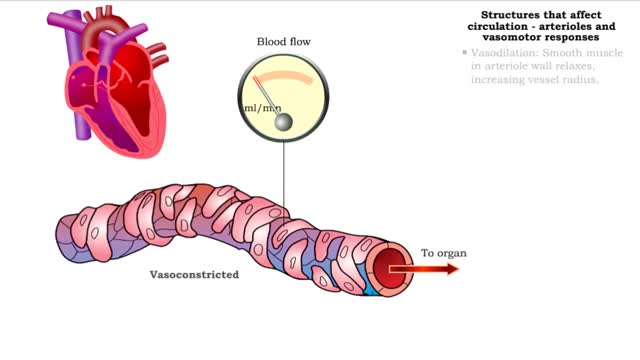
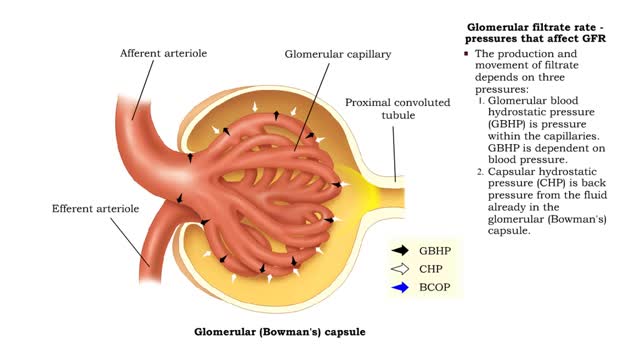
• GFR can be regulated by adjusting: • Blood flow in and out of the glomerular capillaries. • Surface area of glomerular capillaries. • There are three main ways to make these adjustments: • Renal autoregulation. • Nervous regulation. • Renal autoregulation occurs when the kidneys themselves regulate blood flow. • Two renal autoregulatory mechanisms maintain normal GFR over a wide range of systemic blood pressures. • As systemic blood pressure goes up, the smooth muscle cells in the afferent arterioles stretch. • The smooth muscle fibers of the afferent arterioles respond to stretching by contracting, reducing blood flow to the glomerular capillaries. • GFR decreases. • As systemic blood pressure goes down, the smooth muscle cells in the afferent arteriole relax. • The relaxation of the afferent arteriole allows greater blood flow to the capillaries. • GFR increases. Autoregulation via tubuloglomerular feedback Tubuloglornerular feedback. • When blood pressure is above normal, rapid filtrate flow reduces ion retention so filtrate in tubule has more Na+, Cl-, and water. • It is believed that vasoconstricting chemicals from the juxtaglomerular cells are released when the macula densa cells detect higher water and ion levels in the tubule. • These chemicals cause vasoconstriction of the afferent arteriole, thereby reducing blood flow to the glomerular capillaries. • GFR decreases. • Slow filtrate flow increases ion retention so filtrate in the tubule has less Na+, Cl-, and water. • Macula densa cells detect lower water and ion levels in the tubules, inhibiting the release of vasoconstricting chemicals from the juxtaglomerular cells. • The afferent arteriole vasodilates, increasing blood flow to the glomerular capillaries. • GFR increases. Neural regulation • In the case of an extreme drop in blood pressure, sympathetic output increases. • The afferent arterioles vasoconstrict. • The juxtaglomerular cells secrete renin, a chemical that promotes formation of angiotensin II, a potent vasoconstrictor. • The net result of increased sympathetic stimulation is a reduction of blood flow to the glomerular capillaries - a decrease of OFR. • This mechanism eventually reduces urine output, conserving water. Hormonal regulation • If both blood volume and pressure drop, the walls of the renal arterioles collapse. This causes the juxtaglomerular cells to produce renin. • Renin promotes the formation of angiotensin 11. • Increased angiotensin II promotes vasoconstriction of afferent arterioles, reducing blood flow to the glomerular capillaries. • GFR decreases. • A sudden large increase in blood pressure will cause the atria of the heart to stretch. • ANP is released into the bloodstream. • ANP causes the mesangial cells of the glomerulus to relax, increasing the surface area of the capillaries.
Add To
You must login to add videos to your playlists.
Advertisement



Comments
0 Comments total
Sign In to post comments.
No comments have been posted for this video yet.